Long, brutally cold Prairie winters could be masking signs of a serious toxin lurking in livestock producers’ feed bins, a University of Calgary veterinary professor warned feed and livestock industry officials recently.
Dr. Eugene Janzen, assistant dean of clinical practice, said he was initially perplexed in the winter of 2013 when he observed Alberta feedlot cattle in so much distress that it was clear many would have to be euthanized on site.
The feedlot’s cattle had had high rates of severe lameness that didn’t respond to standard treatment for foot rot, as well as unusual degrees of frostbite. Many had frozen ears and an entire pen of heifers had lost the ends of their tails so uniformly that Janzen at first thought they had been surgically removed.
Read Also

First-time pig mothers may need more lysine
Lysine feed recommendations may fall short for gilt pregnancies when it comes to making sure the mother pig can produce as much milk for her piglets as possible
The animals were indeed suffering from frostbite, but it wasn’t because they were poorly sheltered from the winter cold. They had ergot poisoning, which in cattle causes vasoconstriction, or poor blood flow to their extremities. Janzen believes that created a synergistic effect with the cold to cause their symptoms.
Poor blood flow
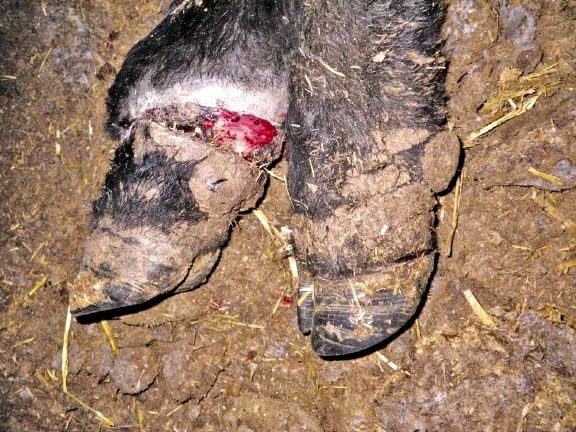
Ergot-affected animals develop “dry gangrene” in their hooves, which can easily be confused with foot rot. “These animals are so lame they don’t lie down naturally,” Janzen said. When they lay with their legs outstretched instead of tucked beneath, their limbs freeze. Several animals he observed could no longer walk.
Janzen was one of the speakers at a symposium on ergot and fusarium at the University of Saskatchewan’s vet college June 12. He said until recently, his own knowledge of ergot was limited to textbook references to a human plague known as Saint Anthony’s Fire in the Middle Ages, and memories of a truckload of durum his father couldn’t sell four decades ago when he was a child on the farm.
But he and other veterinarians across Western Canada have seen a worrisome surge in cases of ergot toxicity in recent years — a phenomenon that has feed manufacturers and grain companies scrambling to develop better guidelines for detection and tolerances.
“It is definitely the No. 1 livestock problem today that is going through our lab,” said Dr. Barry Blakley, a University of Saskatchewan veterinary toxicologist.
Worsening problem
Over the past two decades, it was customary to get calls on one or two cases a year. “Now I am getting four or five calls a day,” he said.

Blakley analyzes the results of feed sample testing provided by the Prairie Diagnostic Services lab at the University of Saskatchewan. The lab installed equipment to test for ergot, beginning in 2013.
- More from the Manitoba Co-operator: Ergot becomes invisible in manufactured feed
Demand for the testing and the diagnostic results suggests ergot has become a much bigger problem in Western Canada than previously thought and that existing guidelines for how much ergot it takes to cause health issues in livestock are seriously outdated.
“Canadian standards through Agriculture Canada are up to 2,000 parts per billion,” he said. “Those are too high. We have seen cases well below that — 700 to 1,600 ppb is the range we’ve seen a lot of cases.”
Saskatchewan has reported the most cases, partly due to growing awareness, but the most severe cases have been seen in Alberta, Blakley said. Only about 10 per cent of the cases he has worked with came from Manitoba, a pocket of cases in the Elm Creek and Ste. Claude area.
Data collected by the Canadian Grain Commission suggests ergot levels haven’t been as high in samples coming from Manitoba. But this province sees a higher incidence of fusarium mycotoxins, such as deoxynivalenol, which also affects feed grain safety.
Industry officials say ergot fungus levels are building in soils across Western Canada due to the rise in zero or minimum tillage and a pattern of moist, cool conditions during June.
New guidelines needed
There are several issues confounding efforts to develop new guidelines.
For starters, there are differences between species and even within species how much the animals can tolerate with no ill effects. For example, only about 10 per cent of the cattle on the Alberta feedlot Janzen visited developed severe symptoms.
“Horses appear to be at the top of the susceptibility chain,” Blakley said. Dairy cows appear more sensitive than beef cows, and sheep have been known to stop milk production at levels of 200 to 300 parts per billion. Results from a swine-feeding trial contradicted earlier research that suggested they were less susceptible. “They are as susceptible if not more susceptible than cattle,” he said.
“The standard we use of 100 to 200 ppb is about as high as you want to go in feed samples,” he said.
Plus, the level of toxicity is affected by the amount of contaminated feed in the ration. The good news is the toxins clear from the animal’s system quickly, and don’t appear to affect the milk or meat. However, that can make it more difficult to identify as the source of an animal’s health problem. “Our diagnostics are basically limited to feed analysis,” Blakley said.
Misdiagnosed
He said most of the cases he’s seen involve cattle producers with subclinical herd health issues that can easily be attributed to other ailments or poor management. Symptoms can include reduced productivity, lower milk production in dairy, a sickly calf crop and low weaning weights. In higher doses, sheep and cattle can suffer abortions and pregnant mares may foal without producing milk.
In the early stages, immediately removing the contaminated feed source can result in full recovery, but once gangrene or frostbite has set in, the producer has few options but to euthanize or sell the animal immediately — if it can be humanely transported.
“It is terribly inhumane. Unless you can call in a mobile butcher, that animal is coyote bait,” Janzen said. “With other diseases, the animal has the decency to die. These animals don’t.”
In the Alberta case, five per cent of the 2,500 head of cattle on the feedlot were destroyed and five per cent were shipped for salvage. “The bottom line is, he went bankrupt.”